What is the most severe type of ichthyosis?
Lamellar ichthyosis, a more severe form of dermatosis, is an autosomal recessive trait with an incidence of 1 case per 300,000 population. X-linked recessive ichthyosis has an incidence of 1 case per 6000 males.
Why do babies with harlequin ichthyosis have red eyes?
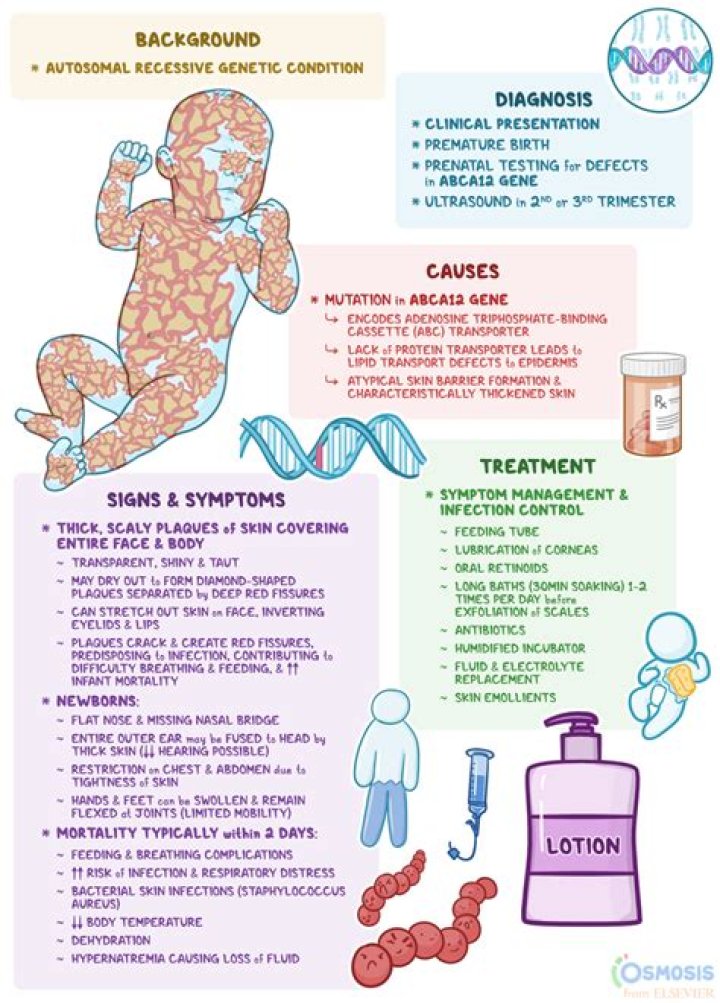
The newborn child is covered with plates of thick skin that crack and split apart. The thick skin plates can pull at and distort facial features. The tightness of the skin pulls around the eyes and the mouth, forcing the eyelids and lips to turn inside out, revealing the red inner linings.
What is the life expectancy of someone with ichthyosis?
People with mild ichthyosis have a normal lifespan. However, the most severe inherited types can be life threatening. If you have inherited ichthyosis, you’ll have it for life. Acquired ichthyosis may get better if the underlying cause is identified and treated.
Is ichthyosis a disability?
Ichthyosis is one of the impairments listed in the Social Security Administrations Blue Book. If your ichthyosis is severe enough (or includes flare-ups that are severe enough) to hinder your ability to work, you may be eligible for Social Security Disability benefits.
Who is the oldest person with harlequin ichthyosis?
The oldest known survivor is Nusrit “Nelly” Shaheen, who was born in 1984 and is in relatively good health as of June 2021.
How long is the average lifespan of a person with ichthyosis?
The prognosis is very poor. Most affected babies do not survive beyond the first week of life. It has been reported that the survival rate varies from 10 months to 25 years with supportive treatment depending on the severity of the condition(8).
Can ichthyosis be cured?
Ichthyosis vulgaris doesn’t have a known cure, so the goal of treatment is to manage the condition.
Is erythroderma genetic?
Congenital ichthyosiform erythroderma is genetically diverse and has been found to have mutations in the same genes as lamellar ichthyosis discussed above (TGM1, ABCA12, ALOXE3, ALOX12B, and NIPAL4) which explains the phenotypic overlap of these two diseases.